Newborn Weight Tool shown to have utility in low- and middle-income countries
(Ginsburg AS et al., Scientific Reports 2023;13:14128 [https://www.nature.com/articles/s41598-023-39773-4])
In a study funded by the Bill and Melinda Gates Foundation, investigators compared weight trajectories in the first 5 days after birth among newborns born in a low- and middle-income countries (LMIC) cohort with those used to develop NEWT. Between April 2019 and March 2020, a convenience sample of 741 singleton healthy breastfeeding newborns who weighed ≥ 2000 g at birth were enrolled at selected health facilities in Guinea-Bissau, Nepal, Pakistan, and Uganda. Using a standardized protocol, newborn weights were obtained within 6 hours of birth and at 1, 2, 3, 4, and 5 days. The trajectories of early newborn weight change in the new cohort were largely similar to those in NEWT, with the exceptions that initial newborn weight loss in Guinea-Bissau was more pronounced than those on NEWT and newborn weight gain following weight nadir was more pronounced in Guinea-Bissau, Pakistan, and Uganda than those in NEWT. The investigators concluded that the data demonstrate that NEWT may have utility in LMIC settings.
Paul recognized for pediatric research excellence
Dr. Ian Paul has been selected for the 2022 American Pediatric Association Research Award, which recognizes an investigator who has advanced pediatric knowledge through excellence in research.
Newborn Weight Tool marks fifth anniversary of helping providers track infant growth
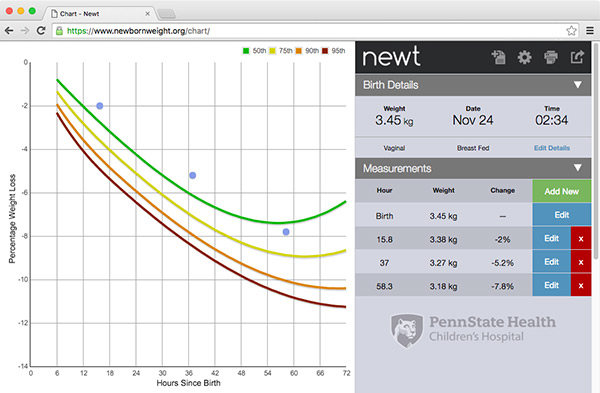
The Newborn Weight Tool (NeWT), developed by Dr. Ian Paul, a pediatrician and professor of pediatrics and public health sciences at Penn State College of Medicine, is enjoying a good measure of online celebrity..
The tool allows providers to compare a newborn’s weight loss against data from more than 160,000 infants. It has earned 2 million page views since it debuted in 2015 and has been used by providers in 179 different nations.
NeWT’s global reach doesn’t surprise Paul, who created the tool with help from Penn State statistician Eric Schaefer and researchers from the University of California, San Francisco and Kaiser Permanente. “Every provider who cares for babies needs this information,” Paul said.
Supplementary Feedings in the Healthy Term Breastfed Neonate
The use of NEWT has been included in the Academy of Breastfeeding Medicine Clinical Protocol #3: Supplementary Feedings in the Healthy Term Breastfed Neonate, Revised 2017. In this protocol, clinicians are encouraged to utilize NEWT to determine the weight loss range for a newborn when considering the need for supplementary feedings.
Newborns often take weeks to return to birth weight
Reuters:
Even though doctors often tell parents that newborns will regain weight lost after birth within a week or two, many infants take much longer to achieve this milestone, a U.S. study suggests.
Nearly all newborns lose weight during the first days after birth, regardless of whether they are breastfed or formula fed. Many doctors expect babies to regain those lost ounces and surpass their birth weight within 10 to 14 days.
But by 14 days, 14 percent of babies born vaginally and 24 percent of infants delivered via cesarean section surgeries didn’t return to their birth weight, the study of almost 144,000 newborns found.
“It is normal for newborns to lose a significant amount of weight in the first 1 to 3 days after delivery due to both urinating excess fluid and limited intake,” said lead study author Dr. Ian Paul, a researcher at Penn State College of Medicine in Hershey, Pennsylvania.
Weight Change Nomograms for the First Month After Birth
Clinicians expect newborns to surpass birth weight by age 10 to 14 days, yet few studies have examined the natural history of weight change in the weeks after birth. We sought to determine the distribution of weight loss and subsequent regain during the first month, the proportion not surpassing birth weight by 14 and 21 days, and whether findings differed by delivery mode.
External Validation of Early Weight Loss Nomograms for Exclusively Breastfed Newborns
Nomograms that show hour-by-hour percentiles of weight loss during the birth hospitalization were recently developed to aid clinical care of breastfeeding newborns. The nomograms for breastfed neonates were based on a sample of 108,907 newborns delivered at 14 Kaiser Permanente medical centers in Northern California (United States). The objective of this study was to externally validate the published nomograms for newborn weight loss using data from a geographically distinct population.
Early Weight Loss Nomograms for Exclusively Breastfed Newborns
The majority of newborns are exclusively breastfed during the birth hospitalization, and weight loss is nearly universal for these neonates. The amount of weight lost varies substantially among newborns with higher amounts of weight loss increasing risk for morbidity. No hour-by-hour newborn weight loss nomogram exists to assist in early identification of those on a trajectory for adverse outcomes.
Early Weight Loss Nomograms for Formula Fed Newborns
Data regarding delivery mode, race/ethnicity, feeding type, and weights were extracted from electronic medical records of the birth hospitalization at 14 Kaiser Permanente Northern California hospitals between 2009 and 2013. Newborns whose first feeding was formula from a cohort of 161471 healthy, term, singleton neonates born at ≥36 weeks’ gestation between 2009 and 2013 were identified. Quantile regression was used to create nomograms stratified according to delivery mode; percentiles of weight loss were estimated as a function of time among formula-fed neonates. Weights measured subsequent to any breast milk feeding were excluded. Percentiles were determined through 48 and 72 hours of age for those born vaginally and via cesarean delivery, respectively.
Study shows some newborns lose weight much faster than previously recognized
Online tool is first to help parents and pediatricians assess newborn weight loss
Using weights obtained from over 100,000 Northern California babies, a new study is the first to detail the weight loss patterns of exclusively breastfed newborns. The results show that some breastfed babies lose weight faster and for a longer period than was previously recognized. Continue reading…